Call 812.424.2020 or 800.489.2020 Fax: 812.424.3000
6149 E. Columbia St. Evansville, IN
Glaucoma
GLAUCOMA
GLAUCOMA
Overview
Overview
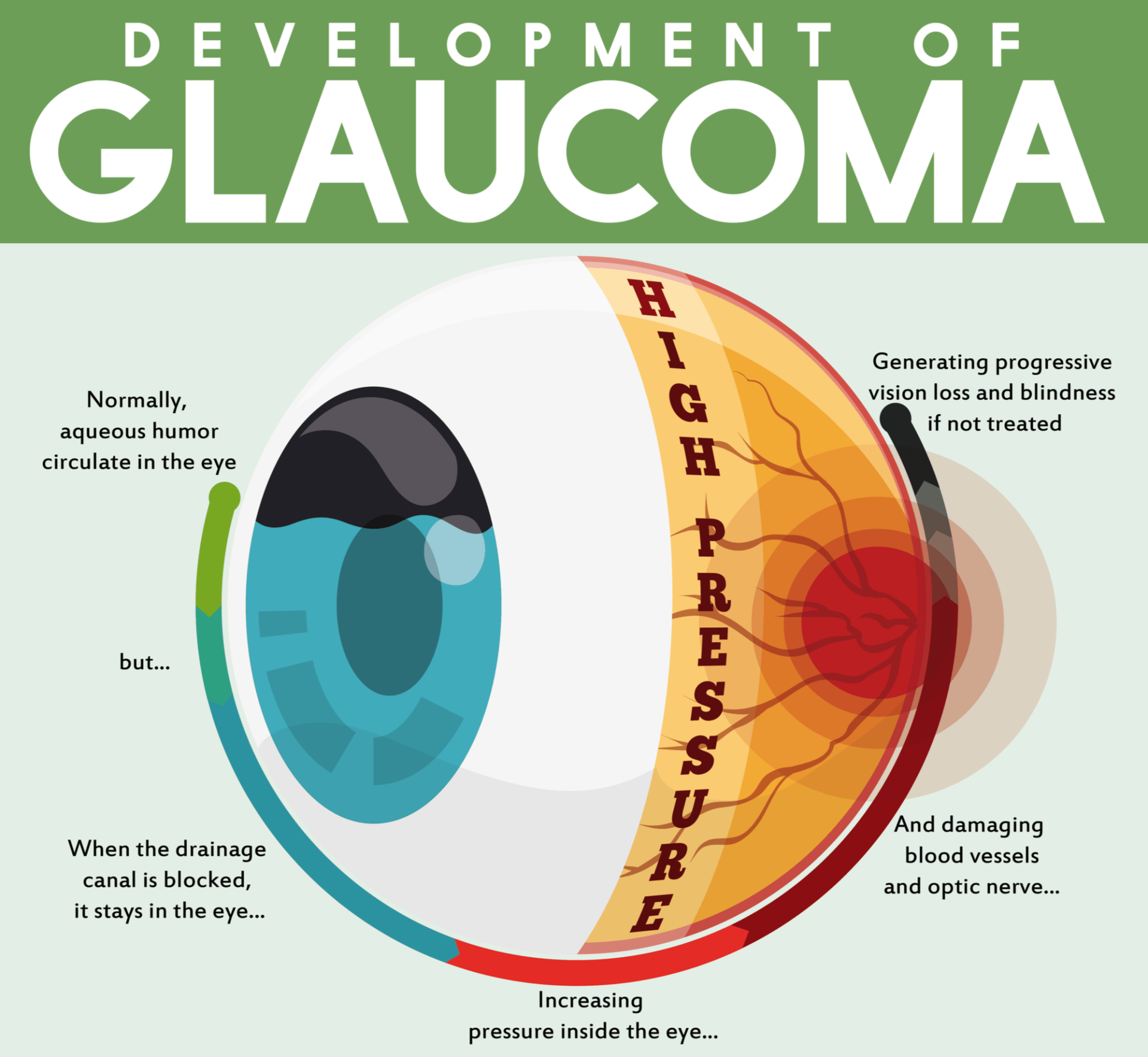
Glaucoma is a group of eye diseases causing optic nerve damage. The optic nerve carries images from the retina, which is the specialized light sensing tissue of the eye, to the brain so we can see. In glaucoma, eye pressure (IOP) plays a role in damaging the delicate nerve fibers of the optic nerve. The higher the IOP, the more likely you are to develop disease and the faster the disease progresses so all treatments for glaucoma are designed to lower the eye pressure. As the optic nerve is damaged, the appearance of the nerve at the back of the eye changes and looks more thinned out. When a significant number of nerve fibers are damaged, blind spots develop in the field of vision. These blind spots can slowly enlarge and impair your overall visual function, even leading to blindness in some cases. Glaucoma is a leading cause of blindness in the world, especially in older people. Although glaucoma is usually treatable, it often does not cause symptoms early on and most people don’t notice these blind areas until much of the optic nerve damage has already occurred. Once vision loss has developed, it is permanent so early detection and treatment by your optometrist or ophthalmologist are the keys to preventing optic nerve damage and vision loss from glaucoma.
What Causes Glaucoma?
The exact causes of optic nerve damage from glaucoma is not fully understood, but involves mechanical compression and/or decreased blood flow of the optic nerve. Although high eye pressure sometimes leads to glaucoma, many people can also develop glaucoma with “normal” eye pressure while many people with higher than average IOP never develop disease. Genetics is thought to play a role as well since glaucoma can run strongly through some families.
Types Of Glaucoma
One of the most confusing aspects of glaucoma for patients is that the term “glaucoma” refers to a number of diseases that all share some common traits but are often caused by different things and even treated differently! The main types of glaucoma are Open Angle Glaucoma (OAG)
and Angle Closure Glaucoma (ACG). In OAG, which is the most common type in the US, the drainage system of the eye appears normal but does not function correctly. This leads to high eye pressure (IOP) and glaucomatous optic nerve damage. There are variants of this as well such as primary open angle glaucoma or POAG (most common type), pigmentary glaucoma, and exfoliative glaucoma. In ACG, which is the most common type in Asia, the drainage system may function correctly but it remains at least partially inaccessible due to blockage by scar tissue or even normal iris tissue as with patients that have very short eyes. This also leads to elevated IOP and glaucomatous nerve damage. Variants of ACG include an anatomic narrow angle, neovascular glaucoma, and phacomorphic glaucoma which is caused by compression of the drainage system by a large cataract.
A special type of ACG is Acute Angle Closure Glaucoma
or Pupil Block Glaucoma. In these cases fluid flow within the eye is sudddenly blocked, causing a rapid rise in IOP that causes eye pain, headaches, nausea/vomiting, eye redness, haloes around lights and blurred vision. If not treated quickly, potentially severe permanent vision loss or even blindness can result. Acute Angle Closure is a medical emergency!
Glaucoma Treatment
As there are many types of glaucoma, there are many treatments available as well. Currently, all glaucoma treatment is geared toward lowering the intraocular pressure (IOP)- but the type of glaucoma often dictates what treatment options are available.
Medication: Topical and oral medications are used to treat all types of glaucoma. These medications reduce the production of fluid within the eye and/or increase the flow of fluid out of the eye in order to reduce IOP.
Laser Surgery: There are three main laser surgeries to treat glaucoma. The first, SLT or Selective Laser Trabeculoplasty, is used to treat the drainage system of the eye to increase fluid flow out of the eye and thus reduce IOP. This is often used for open angle glaucomas. The next, LPI or Laser Peripheral Iridotomy, is used to create a hole in the iris tissue to restore normal fluid flow within the eye. This procedure is reserved for angle closure glaucomas, especially Acute Angle Closure or Pupil Block. The last type is Laser Cyclophotocoagulation or CPC, in which an external laser is used to treat the ciliary body within the eye in order to decrease fluid production and thus lower the IOP. CPC has traditionally been used in severe glaucoma cases but recent advances in laser technology have allowed its use in more mild to moderate cases as welll.
Incisional Surgery: This is usually needed for advanced cases of glaucoma or for those patients who do not respond to medications or lasers. These procedures by-pass the natural drainage system of the eye to allow fluid to pass outside the globe and be absorbed from the external eye tissues, thus lowering the IOP. The main types are Trabeculectomy (or filtering surgery) and insertion of a Glaucoma Tube Shunt. Trabeculectomy is still the “gold standard” of glaucoma procedures to lower IOP and reduce the need for pressure lowering medications.
MIGS (Minimally Invasive Glaucoma Surgery): This group of procedures is newer and although there are many types, most concern either insertion of a shunt into the natural drainage system of the eye (iStent/Hydrus stent) or a partial to total removal of a portion of the drainage system (Trabectome, Kahook blade, Omni system) in order to lower the IOP. These surgeries are usually used in only mild to moderate glaucoma cases and some- like the iStent- can only be done in combination with cataract surgery.
Ancillary Treatments: Some cases of glaucoma are associated with other eye problems and treatment of these conditions can improve the control of the glaucoma itself or improve the chances of glaucoma surgery being successful. For example, neovascular glaucoma is often caused by diabetic retinopathy and control of the retinal process via anti-VEGF drug injections or PRP laser treatment by a retinal disease specialist will improve both IOP control and the likelihood of glaucoma surgery success.
In summary, Glaucoma is a complex set of diseases with many treatment options available. Your eye care provider can educate you about your particular case and advise you as to which treatment options are best for you.
(812) 424-2020
(800) 489-2020
info@talleyeyeinstitute.com
- Mon - Fri
- -
- Sat - Sun
- Closed